The Childhood Cancer Blog
The Childhood Cancer Blog
My time as a writing Intern at Alex’s Lemonade Stand Foundation (ALSF) has been extremely rewarding and educational. I was able to greatly increase my knowledge about copywriting, nonprofits, and the professional world. However, the most eye-opening part of this summer has been a closer glimpse into the world of childhood cancer.
Kicking off
Over winter break, I scoured the internet for an internship that might be even slightly related to writing. In the end, I applied to more than 70 places. I was lucky enough to land a few interviews and even some acceptances, but none... Read More

For children battling this rare brain tumor, treatment options are limited and after relapse, the disease tends to spread quickly.
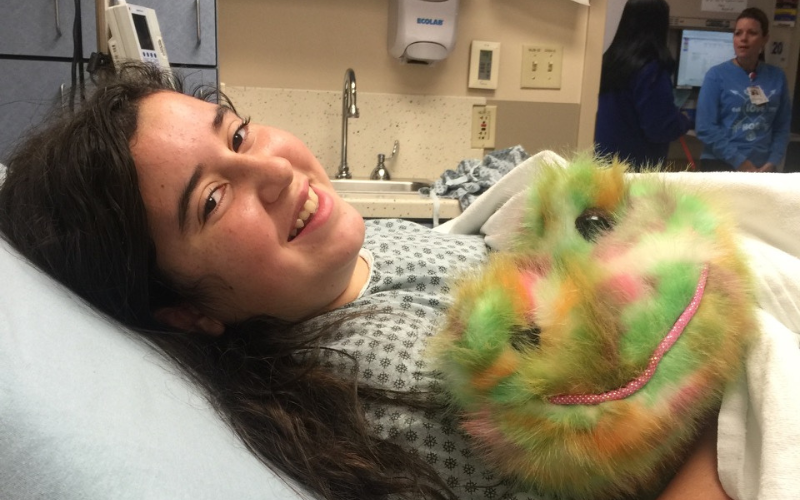
Chloe passed away at 13 years old. Chloe’s mom Michelle desperately searched for a cure for her daughter—and now—she is keeping up the search in memory of Chloe.
While playing goalie for her soccer team in April 2016, Chloe Cox, a super bright 12-year-old from Texarkana, Texas, was kicked in the head. She stood up holding her head, but seemed okay.
In the weeks that followed, Chloe began to have horrible headaches. Her family doctor diagnosed her with a mild concussion, with instructions to return if the headaches continued or got worse. The headaches persisted, and her doctor sent her to the emergency room for a CT scan.
Within one hour, the family had a diagnosis: there was a tumor the size of a walnut near her pineal gland — a... Read More

Above, Crazy 8 Grant teams gathered in Philadelphia in April to share progress on their projects, collaborate, and make valuable connections. Teams traveled from all over the world.
In 2020, ALSF launched its largest, most ambitious grant category ever — the Crazy 8 Initiative. More than just a funding source, the Crazy 8 brings together multi-disciplinary teams from all around the world to study, collaborate, and ultimately make breakthroughs in the search to cure the deadliest childhood cancers. They meet monthly virtually, travel to one another’s labs, and gather in Philadelphia to problem-solve and share progress and technology.
Together, these scientists are making a difference, one incredible discovery at a time.
Several years into their work,... Read More
Pages