Childhood Brain and Spinal Cord Tumors
Long-term side effects
Increasing numbers of children are being cured of their disease and surviving years after a single or tandem PBSCT. The intensity of the treatment prior to, during, and after transplant can cause major effects not apparent for months or years. This section describes a few of the common long-term side effects that sometimes develop after transplant.
Dental development
Certain chemotherapy drugs, administered in high doses prior to transplant, may result in improper tooth development and blunted or absent tooth roots in children who had a transplant when they were younger than 5 years of age. Your child should have a comprehensive dental examination prior to the transplant and a dental follow-up after recovery from the PBSCT.
Thyroid function
Children who receive only chemotherapy do not develop thyroid deficiency as a result of treatment. If, however, your child receives radiation therapy to the brain and spinal cord, either before or following recovery from a transplant, she should be monitored for thyroid deficiency. Tablets containing thyroid hormone are usually effective in treating the problem.
Puberty and fertility
Our 4-year-old son had focal point and cranial/spinal radiation for medulloblastoma and high-dose Cytoxan® for his stem cell transplant. It took about a year for his counts to normalize and he was sick a lot during that time. He takes growth hormone and thyroid replacement. He has severe high frequency hearing loss. But these are nothing compared to the learning difficulties.
If your child receives cranial radiation, either before or following recovery from a transplant, delays in puberty and sexual development can occur. In addition, some of the drugs given in high doses during conditioning (e.g., cyclophosphamide, thiotepa) can cause changes in future fertility (the ability to become a biological parent). For this reason, boys who have gone through puberty should bank sperm before treatment begins. You may also be told about any experimental protocols that are attempting to preserve fertility in girls.
Any child or teen who had a transplant should be followed closely by a pediatric endocrinologist, who can prescribe hormones (testosterone for boys, estrogen and progesterone for girls) to assist in normal pubertal development and can assess fertility in older survivors.
Second cancers
Children who receive a PBSCT have a small risk of developing a second cancer. The risk depends on the chemotherapy drugs given during conditioning. Use of etopoide and cyclophosphamide increases the risk of second cancers.
Because transplants are relatively new treatments for children and teens with brain and spinal cord tumors, the overall impact and long-term effects are not yet clear. Your child’s doctor can explain known risks given your child’s disease and treatment.
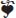
The road of chemotherapy treatment was long and harsh, but transplant was a test of faith and patience. Knowing that Mia’s immune system would be zapped to the point of no return was scary. However, it felt like the last step in killing off any sign of cancer in my little girl’s body and a step closer to the end of this nightmare. Isolation was tough on both of us but once again the staff, the programs, the volunteers, and everyone in the hospital were amazing. Mia’s room was personalized and decorated just for her. She only asked to leave the room the day before we left for good, day 38! The nurses and doctors did everything in their power to make the whole transplant process go as smoothly as possible for all of us. They kept us informed, called us on their days off, helped me clean Mia up when she was sick, and even played dress up to help get her out of bed and shower. We survived, and Mia was discharged on day 39. She walked out dressed like a princess.
We came home on December 10, 2010. Mia has not been admitted since then. What a blessing to be home in time for Christmas. We had spent every holiday in the hospital since Mother’s Day. We were so happy to be home at last and for good! I put the tree up the very next day.
Table of Contents
All Guides- Introduction
- 1. Diagnosis
- 2. The Brain and Spinal Cord
- 3. Types of Tumors
- 4. Telling Your Child and Others
- 5. Choosing a Treatment
- 6. Coping with Procedures
- 7. Forming a Partnership with the Treatment Team
- 8. Hospitalization
- 9. Venous Catheters
- 10. Surgery
- 11. Chemotherapy
- 12. Common Side Effects of Chemotherapy
- 13. Radiation Therapy
- 14. Peripheral Blood Stem Cell Transplantation
- 15. Siblings
- 16. Family and Friends
- 17. Communication and Behavior
- 18. School
- 19. Sources of Support
- 20. Nutrition
- 21. Medical and Financial Record-keeping
- 22. End of Treatment and Beyond
- 23. Recurrence
- 24. Death and Bereavement
- 25. Looking Forward
- Appendix A. Blood Tests and What They Mean
- Appendix C. Books and Websites

